Artificial intelligence (AI) and associated technologies are becoming more common in business and society, and they are beginning to be used in healthcare. Many elements of patient care, as well as administrative operations within providers, payers, and pharmaceutical organizations, have the potential to be transformed by these technologies.
A number of research studies have already found that Artificial Intelligence in healthcare can perform as well as or better than humans in crucial healthcare activities such as illness diagnosis. Algorithms are already surpassing doctors in detecting dangerous tumors and advising researchers on how to build cohorts for expensive clinical trials. However, we anticipate that it will be several years before AI replaces humans in wide medical process areas for a variety of reasons.
Machine Learning
Machine learning is a statistical approach for fitting models to data and teaching models to 'learn' by training them with data. The most prevalent use of classical machine learning in healthcare is precision medicine, which predicts which treatment protocols are likely to be successful on a patient based on numerous patient traits and the treatment environment. Deep learning, or neural network models with many levels of features or variables that predict outcomes, is one of the most advanced kinds of machine learning. There might be thousands of hidden elements in such models that are revealed by the quicker processing of today's graphics processing units and cloud systems. Recognizing possibly malignant tumors in radiography pictures is a typical use of deep learning in healthcare.
Natural Language Processing (NLP)
The most common uses of NLP in healthcare involve the generation, comprehension, and categorization of clinical documentation and published research. NLP systems can analyze unstructured clinical notes on patients, create reports (for example, on radiological exams), transcribe patient conversations, and perform conversational AI.
Rule-based Expert Systems
In the 1980s and beyond, expert systems based on versions of 'if-then' rules were the dominant AI technology in healthcare. To this day, artificial intelligence is routinely employed in healthcare for clinical decision assistance. Many electronic health record systems (EHRs) now provide a set of rules as part of their software offerings.
Human experts and engineers are typically used to create a comprehensive set of rules in a specific knowledge area for expert systems. They work well up to a point and are simple to follow and process. However, once the number of rules increases above a certain threshold, generally several thousand, the rules might begin to clash with one another and break apart.
Robots
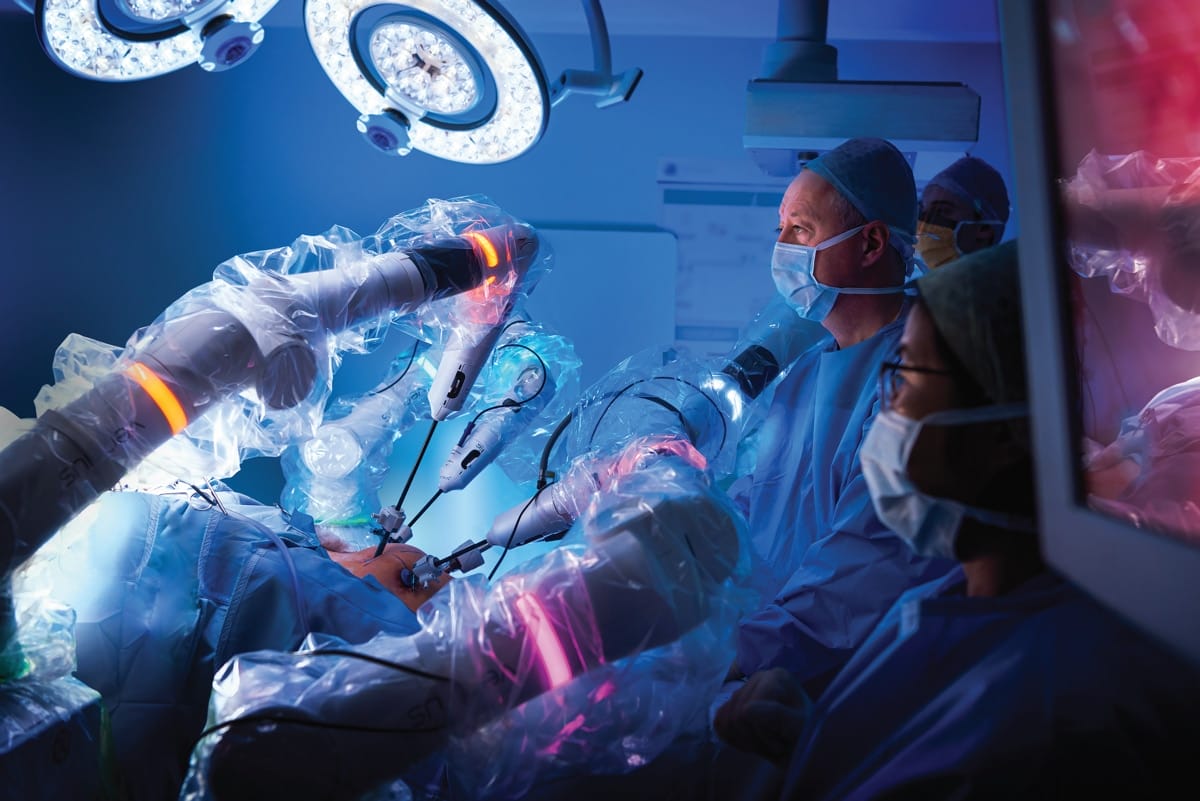
Surgical robots, which were first allowed in the United States in 2000, give surgeons "superpowers" by enhancing their capacity to sight, make accurate and less invasive incisions, suture wounds, and so on. However, important judgments are still made by human surgeons. Gynecologic surgery, prostate surgery, and head and neck surgery are all common surgical procedures that use robotic surgery.
 Diagnosis and Treatment Apps
Diagnosis and Treatment Apps
Since at least the 1970s, when MYCIN was created at Stanford to diagnose blood-borne bacterial infections, illness diagnosis and treatment have been a focus of AI. This and other early rule-based systems had promised to properly identify and treat disease but were not accepted for practical use. IBM's Watson has gotten a lot of press for its emphasis on precision medicine, notably cancer detection and treatment. Watson makes use of a combination of machine learning and natural language processing (NLP). However, customers' enthusiasm for this use of the technology has waned as they realized how difficult it is to train Watson how to handle specific forms of cancer and integrate Watson into care procedures and systems.
The Ethical Aspect
There are also other ethical issues associated with the usage of AI in healthcare. In the past, practically all healthcare choices were made by people, and the use of smart computers to make or help with them poses questions of responsibility, transparency, consent, and privacy. Many AI systems, particularly deep learning algorithms used for image analysis, are very hard to understand or comprehend. If a patient is told that a picture has led to a cancer diagnosis, he or she would most certainly want to know why. Deep learning algorithms, and even doctors who are familiar with their functioning, may be unable to give an explanation.
The Future of AI in Healthcare
The most difficult hurdle for AI in many healthcare fields is guaranteeing their acceptance in everyday clinical practice, not whether the technologies will be capable enough to be useful. These problems will be addressed in the end, but it will take considerably longer than the technologies themselves to mature. As a result, we anticipate limited application of AI in clinical practice during the next five years, followed by more widespread usage within the next decade. It also appears evident that AI systems will not replace human physicians on a big scale, but will rather supplement their efforts to care for patients.
You can also check out
How Do Smart Devices Improve People's Health
Why Should You Know About the Apple iOS 15.4.1 Update
The Sci-Fi Looking Headphone from Dyson Zone Is Actually an Air Purifier
We hope you love our reviews! For your information, we do earn money from commission in the link in the content! For more information click here!
















